Get Easy Health Digest™ in your inbox and don’t miss a thing when you subscribe today. Plus, get the free bonus report, Mother Nature’s Tips, Tricks and Remedies for Cholesterol, Blood Pressure & Blood Sugar as my way of saying welcome to the community!
Lyme disease is America’s secret silent plague
People experiencing a range of symptoms like fatigue, headaches, poor memory, inability to concentrate, depression, anxiety, recurrent flu-like symptoms, rashes and a general sense of not feeling well may have conditions that are not always easily diagnosed by doctors. Lyme disease is one such illness.
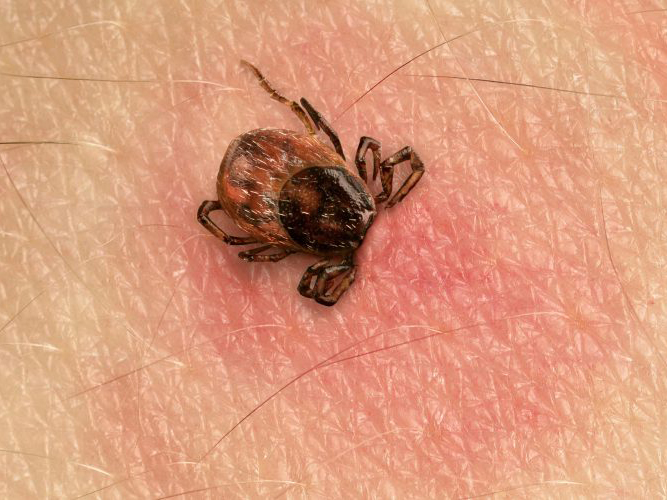
Lyme disease is caused by the bacterium Borrelia burgdorferi and is transmitted through the bite of infected blacklegged ticks (deer ticks) inhabiting deciduous forests through the Northeastern and Southeastern U.S. and in the upper Midwestern states.
Lyme disease produces a host of symptoms including fever, chills, headache, fatigue, muscle and joint aches, swollen lymph nodes, facial palsy, swollen joints and rash which begin within 3 to 30 days after the tick bite.
People may have Lyme disease and not test positive for it; others who do test positive did not suspect it or can’t recall being bitten by a tick. Lyme disease can overlap with other conditions such as chemical sensitivity, viral infections, bacterial infections and mold.
Even years after being diagnosed, up to two out of 10 treated patients suffer from symptoms such as muscle and joint pains, cognitive defects, sleep disturbance and fatigue for months and even years.
It could be the persistent infection or it could be the autoimmune response, where your own immune system damages the body’s tissues by continuing to respond even after the infection has been eliminated.
The Centers for Disease Control and Prevention says that there are between 25,000 and 30,000 cases of Lyme disease officially recorded each year. But it admits those numbers may represent only 10 percent of actual incidences of the disease.
The normal treatment is standard medicine’s typical treatment – antibiotics. But many people do not want to take them anymore, and many also now do not respond to them at all. And since there is not a one-size-fits-all approach in the management of Lyme disease, I will share with you the advice and research of Dr. Nafysa Parpia of the Amitabha Clinic who specializes in Lyme disease, cancer, autoimmune disease and environmental toxicity.
Foundational support
It is critical to have (as stable as possible) a foundation of health before beginning the intense treatment that chronic Lyme requires.
Many Lyme patients are nutrition savvy; however, they still may not be eating a diet that is appropriate for their particular constitution. It is possible that their diet may not be targeted to optimize the body’s detoxification systems and cellular biochemical reactions.
Sensitivity or allergic reaction to foods consumed by the patient may be creating more inflammation in the body. They may not be consuming adequate levels of micro- and macronutrients.
Special laboratory work can reveal genetic tendencies or specific imbalances in the body’s natural biochemical makeup. People with Lyme disease often have these imbalances that need to be addressed in order for healing to be optimized.
Elimination of toxins
Lyme disease patients are more susceptible to illness from toxin exposure as their immune systems are already weakened. In addition, they will not receive the full benefit of treatment from antibiotics, herbal and nutritional therapies when toxic burdens to the body are high. Therefore, a detoxification protocol is key in the treatment of Lyme disease. Detoxification could include heavy metal chelation, neural therapy and strengthening of the liver’s natural detoxification pathways.
Regular sweating is important as well for the excretion of toxic substances.
Nutrients, herbs and supplementation are also given to support all the organs of elimination.
Lyme patients very often benefit from intravenous therapy with micronutrients, glutathione and phosphatidylcholine.
Phosphatidylcholine helps remove toxins from the nervous system, while glutathione flushes them from the body.
Microbes and biofilm
Co-infections and opportunistic infections in Lyme patients are common. Microbes exist in communities: bacteria, viruses, mycoplasma and molds cohabitate, and it is very common for Lyme patients to suffer from a variety of these. Microbes secrete biotoxins to subdue the host’s immune responses. Therefore, treatment with antibiotics and/or herbal antimicrobials to address these coinfections is indeed sometimes warranted.
As Lyme is a multi-systemic disease, treatment needs to be comprehensive and individualized.
Protocols must address not only support of the organs and the body’s natural biochemical processes, but also safe detoxification.












