Get Easy Health Digest™ in your inbox and don’t miss a thing when you subscribe today. Plus, get the free bonus report, Mother Nature’s Tips, Tricks and Remedies for Cholesterol, Blood Pressure & Blood Sugar as my way of saying welcome to the community!
Cholesterol and heart disease: Prepare to be mind-blown
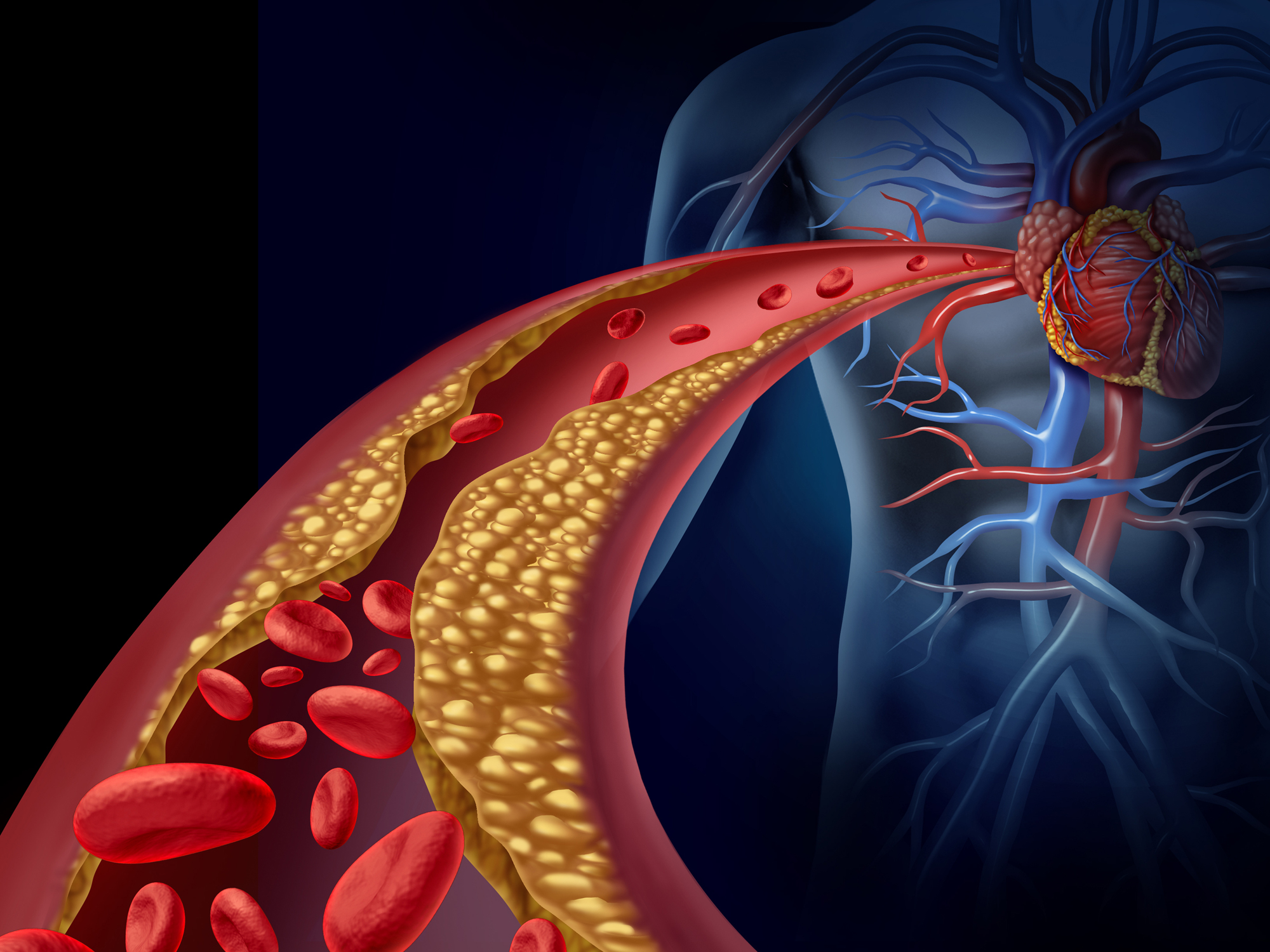
As you probably know, testing for cholesterol has been the standard blood test to evaluate your risk for heart disease for decades.
But when we look at all the data, we find cholesterol itself is not even a real cause of heart disease. In this article, I’d like to tell you the truth about cholesterol blood tests and heart disease risk factors.
LDL-Cholesterol very poorly correlates with heart attack risk
Because cholesterol doesn’t dissolve in your blood, it must be transported by carrier molecules that are water-soluble. These carrier molecules are called lipoproteins. Lipoproteins are made of fat (lipid) and proteins.
The two main types of lipoproteins that transport cholesterol in your bloodstream are:
- High-density lipoprotein or HDL-cholesterol (a.k.a. HDL-C): This has been called the “good” cholesterol because it helps keep cholesterol from becoming arterial plaque.
- Low-density lipoprotein or LDL-cholesterol (a.k.a. LDL-C): This has been called your “bad” cholesterol because this had for years been correlated with higher risk for heart disease. It was postulated to build up in your arteries—forming plaque that narrows and stiffens your arteries.
You’ll also see cholesterol test results with the following along with HDL-C and LDL-C:
- Triglycerides: Elevated levels of this fat have been linked to insulin resistance, diabetes, and indirectly to heart disease. Triglyceride levels rise from eating too many grains and other foods that quickly turn into sugar in your bloodstream. Also, the trend higher if you are sedentary, smoke cigarettes, drink alcohol excessively, or are overweight.
Cholesterol is not the cause of heart disease
Now, what if I told you that having elevated LDL-C cholesterol is a rather poor predictor of heart attack? It’s true. When you look at all the data, we find cholesterol itself is likely not the cause of heart disease, even though there have been correlations.
Here are essential studies which tell us more of the story about cholesterol itself – that it is not what causes heart disease…
- A 1964 report in the Journal of the American Medical Association (JAMA) was published by the famous heart surgeon, Dr. DeBakey. He reported on 1,700 of his surgical patients and found no correlation between blood cholesterol levels and the severity of coronary artery disease discovered during his open heart surgeries.
- The Framingham Study followed 5209 men and women, selected randomly from 10,000 men and women residents living in the town in 1948, who were between the ages of 30 and 62. At the beginning of the study, 5127 were free of cardiovascular disease. In 1977 researchers examined blood cholesterol levels of 2,815 men and women aged 49 to 82 years and reported that “the major potent lipid risk factor was HDL cholesterol,” and that “Total cholesterol was not associated with the risk of coronary heart disease.”
- In 1992 researchers reported further information about cholesterol and heart disease in these same Framingham study participants, then passing through older age. They found that “the total cholesterol-HDL cholesterol ratio is the only lipid attribute that discriminates in a statistically significant way CHD-free survival time in men 65 or older.”
- In 1997 the Lancet reported a study of 724 participants and found that high total cholesterol concentrations were associated with longevity in people older than 85 years, owing to lower death rates from cancer and infection.
- Researchers at Yale University, in a 1994 JAMA article, summarized their report by stating, “Our findings do not support the hypothesis that hypercholesterolemia or low HDL-C are important risk factors for all-cause mortality, coronary heart disease mortality, or hospitalization for myocardial infarction or unstable angina in this cohort of [997] persons older than 70 years.”
- A 2004 Lancet study tallied information from 15,152 people who have had a heart attack and 14,820 control patients in 52 different countries, looking at smoking, history of hypertension or diabetes, waist/hip ratio, dietary patterns, physical activity, consumption of alcohol, blood apolipoproteins (Apo), psychosocial factors, daily consumption of fruits and vegetables, regular alcohol consumption, and regular physical activity. They found that collectively, these nine risk factors accounted for 90% of the attributable risk for heart attack in men and 94% of the risk in women.
- A landmark study in 2009 revealed that nearly 75% of patients who are hospitalized for a heart attack have LDL cholesterol levels within the recommended target for LDL cholesterol.
- Eating more cholesterol does not increase your risk of heart attack. In only about 25% of us, dietary cholesterol modestly increases LDL-C and HDL-C but still it does not affect our LDL to HDL ratio or increase heart disease risk.
- While short-term studies show a relationship between saturated fat intake and blood cholesterol levels, nearly all the long-term studies do not show this.
- A huge prospective meta-analysis reported in 2010 involving nearly 350,000 people found no association between saturated fat and heart disease. And, a Japanese study of 58,000 men followed for 14 years (on average) found no association between saturated fat intake and heart disease; those who consumed more saturated fat had a lower stroke risk.
- Similar rates of heart attack and overall death occur equally in groups who lowered their cholesterol compared to groups who did not, according to the results of more than 40 different clinical trials.
What if the association between LDL-C and heart disease that has been reported in other large studies is due to the presence of cholesterol repairing lesions in your arteries? From this perspective, LDL-C would be a measure of the damage that has already occurred. Cholesterol is not the real villain.
Yet, mainstream medicine continues to focus on the need for a drug to lower LDL-C and warns against saturated fat. We know that statin drugs do lower heart disease and they lower LDL-C… but they also raise HDL-C. Now millions of people (nearly 1 in 4 Americans over age 45) are prescribed statins to lower their cholesterol. And the worry has been all about “elevated cholesterol.” Cholesterol is not the real villain here.
The real villain is the combination of other modifiable causes (you can change 90% of them through lifestyle) which trigger inflammation in your body. With this inflammation, your cholesterol becomes sticky and then becomes part of an atherosclerotic plaque.
Instead of measuring cholesterol and then taking drugs to lower your cholesterol, you will far more effectively reduce your risk of heart attack by eliminating all these other risk factors which make cholesterol sticky. Remember, it’s the atherosclerotic plaque that you don’t want…not low cholesterol. In fact, the higher your HDL-C the lower your risk for heart disease. Maybe you will consider supplements that boost your HDL-C such as omega-3 oils in your diet and niacin, along with other heart-healthy supplements, which I’ll discuss in a near future article.
In my next article, I’ll explain some newer blood tests that are more predictive of your heart attack risk than LDL-Cholesterol.
Editor’s note: While you’re doing all the right things to protect your brain as you age, make sure you don’t make the mistake 38 million Americans do every day — by taking a drug that robs them of an essential brain nutrient! Click here to discover the truth about the Cholesterol Super-Brain!
Sources:
-
http://www.heart.org/HEARTORG/Conditions/Cholesterol/AboutCholesterol/Good-vs-Bad-Cholesterol_UCM_305561_Article.jsp#.WAUNBOArLHo
-
DeBakey, Michael: JAMA 189:655, 1964
-
Gordon T, Castelli WP, Hjortland MC, Kannel WB, Dawber TR. High density lipoprotein as a protective factor against coronary heart disease. The Framingham Study. Am J Med. 1977 May;62(5):707-14. PubMed PMID: 193398. Find online at: https://www.ncbi.nlm.nih.gov/pubmed/193398/
-
William P. Castelli, MD, Keaven Anderson, PhD, Peter W. F. Wilson, MD, and Daniel Levy, MD. Lipids and Risk of Coronary Heart Disease The Framingham Study. AEP Vol. 2, No. l/2 January/March 1992: 23-28. Find online at: https://eurekamag.com/pdf.php?pdf=002424191
-
Weverling-Rijnsburger AW, Blauw GJ, Lagaay AM, Knook DL, Meinders AE, Westendorp RG. Total cholesterol and risk of mortality in the oldest old. Lancet. 1997 Oct 18;350(9085):1119-23. Find online at: https://www.ncbi.nlm.nih.gov/pubmed/9343498
-
Krumholz HM, Seeman TE, Merrill SS, Mendes de Leon CF, Vaccarino V, Silverman DI, Tsukahara R, Ostfeld AM, Berkman LF. Lack of association between cholesterol and coronary heart disease mortality and morbidity and all-cause mortality in persons older than 70 years. JAMA. 1994 Nov 2;272(17):1335-40. Find online at: https://www.ncbi.nlm.nih.gov/pubmed/?term=Lack+of+Association+Between+Cholesterol+and+Coronary+Heart+Disease+Mortality+and+Morbidity+and+All-cause+Mortality+in+Persons+Older+Than+70+Years
-
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, McQueen M, Budaj A, Pais P, Varigos J, Lisheng L; INTERHEART Study Investigators. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet. 2004 Sep 11-17;364(9438):937-52. PubMed PMID: 15364185. Found online at: https://www.ncbi.nlm.nih.gov/pubmed/15364185
-
Sachdeva A, Cannon CP, Deedwania PC, Labresh KA, Smith SC Jr, Dai D, Hernandez A, Fonarow GC. Lipid levels in patients hospitalized with coronary artery disease: an analysis of 136,905 hospitalizations in Get With The Guidelines. Am Heart J. 2009 Jan;157(1):111-117.e2. Online at: https://www.ncbi.nlm.nih.gov/pubmed/?term=136%2C905+patients%2C+2000+and+2006
-
Djoussé L, Gaziano JM. Dietary cholesterol and coronary artery disease: a systematic review. Curr Atheroscler Rep. 2009 Nov;11(6):418-22. Review. PubMed PMID: 19852882. Find online at: https://www.ncbi.nlm.nih.gov/pubmed/19852882
-
https://wholehealthsource.blogspot.com/2011/01/does-dietary-saturated-fat-increase.html
-
Siri-Tarino PW, Sun Q, Hu FB, Krauss RM. Meta-analysis of prospective cohort studies evaluating the association of saturated fat with cardiovascular disease. Am J Clin Nutr. 2010 Mar;91(3):535-46. PubMed PMID: 20071648. Find online at: https://www.ncbi.nlm.nih.gov/pubmed/20071648?dopt=AbstractPlus
-
Yamagishi K, Iso H, Yatsuya H, Tanabe N, Date C, Kikuchi S, Yamamoto A, Inaba Y, Tamakoshi A; JACC Study Group. Dietary intake of saturated fatty acids and mortality from cardiovascular disease in Japanese: the Japan Collaborative Cohort Study for Evaluation of Cancer Risk (JACC) Study. Am J Clin Nutr. 2010 Oct;92(4):759-65. Find online at: https://www.ncbi.nlm.nih.gov/pubmed/20685950?dopt=AbstractPlus
-
http://www.naturalnews.com/025891_cholesterol_high_disease.html
-
Mercola J., “5 Great Reasons Why You Should Not Take Statins,” retrieved 05/03/2016 from http://articles.mercola.com/sites/articles/archive/2016/02/10/5-reasons-why-you-should-not-take-statins.aspx
-
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, McQueen M, Budaj A, Pais P, Varigos J, Lisheng L; INTERHEART Study Investigators. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet. 2004 Sep 11-17;364(9438):937-52. PubMed PMID: 15364185. Found online at: https://www.ncbi.nlm.nih.gov/pubmed/15364185













