Get Easy Health Digest™ in your inbox and don’t miss a thing when you subscribe today. Plus, get the free bonus report, Mother Nature’s Tips, Tricks and Remedies for Cholesterol, Blood Pressure & Blood Sugar as my way of saying welcome to the community!
What hot flashes predict about sleep apnea
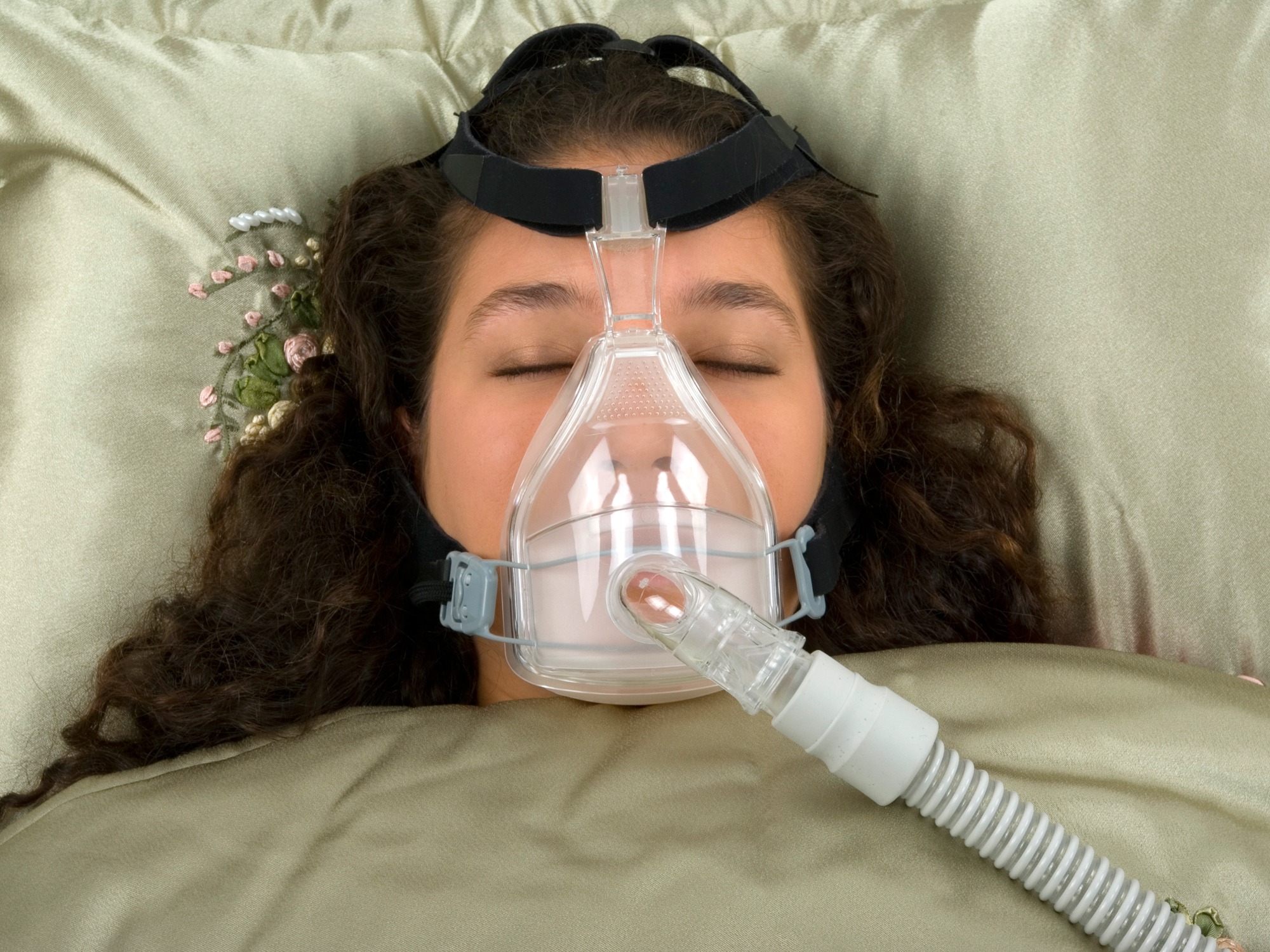
Obstructive sleep apnea (OSA) is a sleep disorder where your throat muscles sporadically relax during sleep and temporarily block your airway.
In men, obstructive sleep apnea is pretty easy to spot, because men with this sleep disorder usually snore like a buzz saw.
But women with obstructive sleep apnea don’t necessarily snore. Their symptoms are more subtle. They deal with insomnia, headaches, fatigue, depression and anxiety. And all of these symptoms are easily overlooked or attributed to another cause (like menopause).
In addition to the fact that women have less obvious obstructive sleep apnea symptoms, menopausal women also have a bunch of risk factors that make them more likely to develop the condition…
Is something more sinister stealing your sleep?
A recent study published in the journal Menopause found that women who are older, have a higher body mass index and have hypertension were more likely to develop obstructive sleep apnea — and these characteristics apply more to menopausal women.
This study had another interesting finding…
Hot flashes don’t just contribute to sleep problems because they’re so darn uncomfortable. They also put you at a higher risk for sleep disorders like OSA. Researchers in the study found that women with severe hot flashes were 1.87 times more likely to have obstructive sleep apnea than women with mild hot flashes or no hot flashes.
“Sleep disruption is a common complaint at menopause. It is important to recognize the high number of undiagnosed sleep disorders, including OSA,” says Dr. JoAnn Pinkerton, The North American Menopause Society executive director. “Early morning headaches or excessive daytime sleepiness should raise concern for obstructive sleep apnea and signal a possible need for sleep apnea testing.”
So the message here is, there’s more to the story if you’re a menopausal woman struggling with sleep issues. Even if you think your hot flashes are to blame for your lack of sleep, you may want to stay alert for symptoms of obstructive sleep apnea just in case. These symptoms include fatigue, insomnia, restless legs, depression, nightmares, palpitations and headaches.
Obstructive sleep apnea, after all, is more than just exhausting and annoying. It can even be deadly, since it increases your chance of sudden cardiac death. So now is the time to get your sleep issues sorted out.
Putting a stop to OSA-related sleep issues
If you notice symptoms similar to those mentioned above, ask your doctor to test you for sleep apnea. Usually, that involves you relaying your symptoms in detail, receiving a physical exam to check for any structural blockages and participating in a sleep study that measures how well you sleep.
If you have obstructive sleep apnea, your best bet is to invest in a continuous positive airway pressure (CPAP) machine, a machine that blows compressed air into your airway while you sleep to keep it open.
Of course, if your obstructive sleep apnea is mild, you can try lifestyle changes first, like:
- Losing weight (if you’re overweight)
- Exercising
- Avoiding alcohol, tranquilizers and sleeping pills
- Sleeping on your side or stomach instead of your back
- Using nasal spray, nasal decongestants or antihistamines to keep your nose from getting stuffy
Editor’s note: What do you really know about stroke? The truth is, only 10% of stroke survivors recover almost completely, and all doctors can offer is what to do after a stroke occurs. That’s unacceptable considering 80% of strokes are preventable! Click here to discover how to escape The Stroke Syndrome: 5 Signs it’s Stalking You — Plus the Hidden Causes and Preventive Measures You’ve Never Heard About!
Sources:
- Obstructive Sleep Apnea — Mayo Clinic. Retrieved November 1, 2017.
- New study links severe hot flashes with greater risk of obstructive sleep apnea — MedicalXpress. Retrieved November 1, 2017.
- Obstructive Sleep Apnea Raises Sudden Cardiac Death Risk — Medical News Today. Retrieved November 1, 2017.
- Wimms, et al. “Obstructive Sleep Apnea in Women: Specific Issues and Interventions.” — Biomed Research International. 2016.
- How Is Sleep Apnea Diagnosed? — National Heart Lung and Blood Institute. Retrieved November 1, 2017.














